Imagine living with a mind that never truly goes quiet – where one thought races ahead while another gets stuck in a loop.
For many people living with both ADHD and OCD, daily life can feel emotionally exhausting in ways that are difficult to explain. Racing thoughts, intrusive fears, mental noise, overthinking, impulsivity, and rumination often blur together over time, especially after years of going undiagnosed or misunderstood. What many people experience is not simply distraction or worry, but a constant internal battle between urgency and repetition, chaos and control.
Why ADHD and OCD Are Often Confused
Although Attention-Deficit/Hyperactivity Disorder and Obsessive-Compulsive Disorder are very different conditions, the overlap in concentration difficulties, restlessness, routines, and overthinking can make them difficult to recognise apart.
Many people spend years feeling misunderstood because symptoms overlap in ways that are easy to misread – by professionals, families, workplaces, and even by the person themselves.
Both can affect concentration, routines, emotional regulation, sleep, decision-making, and daily functioning. Someone with ADHD may appear restless, distracted, forgetful, or unable to finish tasks. Someone with OCD may also struggle to focus, especially when intrusive thoughts, compulsions, or mental rituals take over their attention.
This overlap can make diagnosis complicated. For example:
- A person with ADHD may repeatedly check things because they genuinely forget.
- A person with OCD may repeatedly check things because of anxiety and intrusive fears.
- ADHD can lead to disorganisation and unfinished tasks.
- OCD can lead to perfectionism and fear of making mistakes, which may also stop tasks from being completed.
From the outside, both experiences can look almost identical.
The Paradox of Cooccurrence: “Chaotic” ADHD and “Orderly” OCD
ADHD and OCD can overlap in ways that feel confusing, exhausting, and at times contradictory. Although they are often viewed as being on opposite ends of the spectrum, many people live with traits of both at the same time. Fast, racing thoughts can exist alongside repetitive fears and compulsions. A need for stimulation can clash with a strong need for control. Because of this overlap, one condition is sometimes missed, misunderstood, or diagnosed much later in life, leaving people struggling for years without clear answers.
Many people describe receiving an ADHD and OCD dual diagnosis as a huge relief. Thoughts, behaviours, and struggles that felt confusing for years finally begin to make sense. For the first time, many people feel understood instead of judged, while also gaining access to the right support, therapy, and coping strategies that can genuinely improve quality of life.
Around 30% of people with Obsessive-Compulsive Disorder are also estimated to have Attention-Deficit/Hyperactivity Disorder, with the overlap affecting children, young people, and adults in ways that are often misunderstood or missed for years.

How ADHD and OCD Interact
With ADHD, difficulties are often linked to executive functioning – attention regulation, impulsivity, time management, and task initiation. The brain may constantly seek stimulation, jump between thoughts, or struggle to prioritise information.
With OCD, the experience is usually driven by distressing intrusive thoughts and compulsions aimed at reducing anxiety or preventing something feared from happening. Many people describe feeling trapped in repetitive mental loops that are exhausting and difficult to control.
A person can also live with both conditions at the same time. In these cases, symptoms may interact in confusing ways:
- ADHD impulsivity can intensify compulsive behaviours
- OCD perfectionism can clash with ADHD disorganisation
- Constant mental noise can make it difficult to separate intrusive thoughts from racing thoughts
- Emotional exhaustion often builds over years of masking, self-blame, or missed diagnosis
Commonly Overlapping OCD Symptoms
Some Obsessive-Compulsive Disorder symptoms that are sometimes confused with ADHD include:
- Repetitive checking
- Difficulty concentrating due to intrusive thoughts
- Mental rumination
- Need for reassurance
- Difficulty completing tasks
- Restlessness caused by anxiety
- Overthinking conversations or mistakes
- Repeating routines or rituals to reduce distress
When both are present, they can create a cycle where each condition keeps triggering the other:
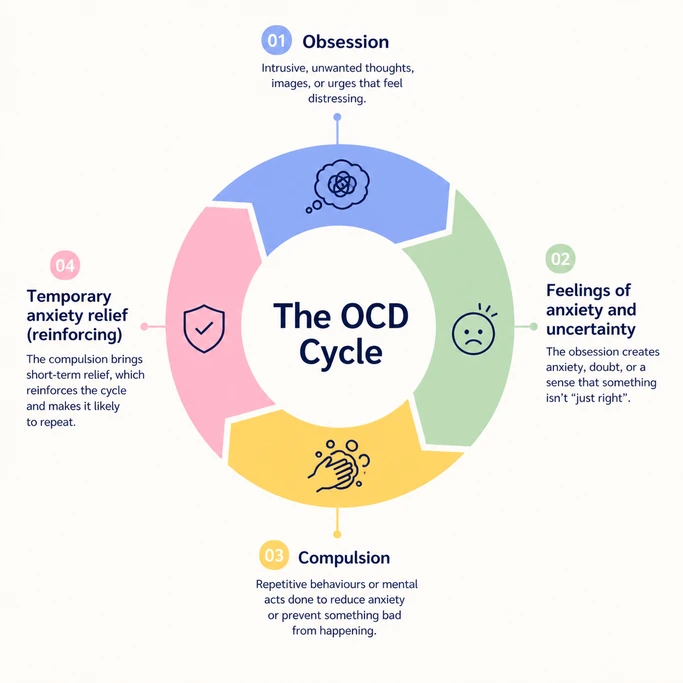
Executive Functioning Struggles
ADHD forgetfulness or distraction can increase OCD anxiety.
Example: someone with ADHD may forget whether they locked the door or completed a task properly. OCD then steps in with repeated checking, reassurance seeking, or mental reviewing.
Hyperfocus vs. Obsession
Hyperfocus and rumination can become hard to separate.
ADHD hyperfocus may lock onto a thought or task for hours, while OCD rumination keeps the brain trapped in repetitive fear loops. Many people describe feeling mentally “stuck.”
The Anxiety Loop
ADHD symptoms such as forgetfulness, disorganisation, missed deadlines, or difficulty staying on top of daily tasks can create constant anxiety and uncertainty. For some people, OCD behaviours develop as an attempt to regain a sense of control or certainty. Rechecking, rigid routines, reassurance seeking, or mental reviewing may temporarily reduce anxiety, but over time the cycle often becomes exhausting and difficult to break.
When OCD Makes ADHD Paralysis Worse
Compulsions, rumination, and perfectionism can consume so much mental energy that focus, planning, decision-making, and task completion become even more difficult. Many people describe feeling overwhelmed before they have even started a task.
Impulsivity, Guilt, and OCD Fears
ADHD impulsivity, such as interrupting, blurting things out, forgetting details, or acting quickly, can trigger obsessive guilt and overthinking. A person may repeatedly replay conversations or fear they have done something wrong, even when others have moved on.
Perfectionism vs. Executive Dysfunction
OCD may create a strong need for things to feel “perfect,” organised, or completed in an exact way, while ADHD can make starting tasks, prioritising, or maintaining attention difficult. This clash often leads to frustration, self-criticism, avoidance, and burnout.
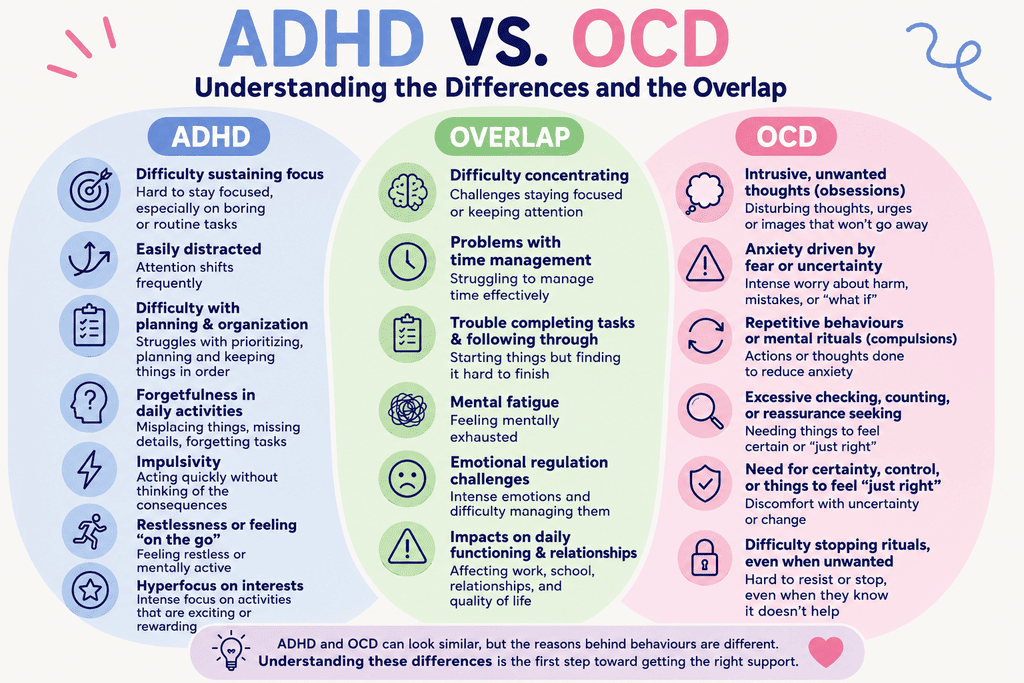
Distinguishing the Symptoms: ADHD vs. OCD
One person may struggle with focus because their brain constantly shifts attention, while another may feel trapped in repetitive thoughts, difficulty focusing and rituals driven by anxiety and fear. This overlap can make it difficult for people to understand what they are experiencing, especially when both conditions exist together. Understanding the difference is an important step toward finding the right support, coping strategies, and answers that many people spend years searching for.
Research has also shown differences in how the brain functions in each condition. Although ADHD and OCD both involve the frontostriatal circuit – an area linked to attention, decision-making, impulse control, and behaviour regulation – brain imaging studies have found very different patterns.
People with ADHD often show lower activity in these areas, which can affect focus, organisation, and impulse control. In OCD, the same circuit is often overactive, contributing to intrusive thoughts, repetitive behaviours, and heightened anxiety.
ADHD Core Traits
- Difficulty maintaining focus, especially on tasks that feel repetitive or unstimulating
- Executive functioning challenges, including planning, organisation, time management, and task completion
- Forgetfulness and distractibility in daily activities
- Impulsivity, such as interrupting, acting quickly, or making rushed decisions
- Restlessness or feeling mentally “on the go”
- Hyperfocus on interests or activities that feel rewarding or stimulating
OCD Core Traits
- Intrusive, unwanted thoughts, fears, or mental images (obsessions)
- Persistent anxiety linked to uncertainty, fear, or a sense that something feels “wrong”
- Repetitive behaviours or mental rituals (compulsions) carried out to reduce distress
- Excessive checking, reassurance seeking, counting, repeating, or reviewing thoughts
- Strong need for certainty, control, or things feeling “just right”
- Difficulty stopping rituals even when the person knows they may not make logical sense
Where It Can Feel Confusing
- ADHD distraction can look like avoidance
- OCD rumination can look like hyperfocus
- ADHD impulsivity may increase OCD fears or self-doubt
- Both can affect concentration, routines, emotional regulation, and daily functioning
- Many people describe feeling mentally exhausted from constantly battling their own thoughts
The Challenge of Diagnosis: “Masking” and Misdiagnosis
ADHD and OCD are two different disorders, but their overlapping symptoms can make diagnosis more complex. A person may appear organised, careful, or “high-functioning” on the outside, while internally they are relying on OCD compulsions to manage fear, uncertainty, or intrusive thoughts.
For example, repeated checking, list-making, cleaning, arranging, or reassurance-seeking may look like strong organisation. In reality, these behaviours may be driven by anxiety and a need to neutralise obsessive thoughts. At the same time, ADHD-like symptoms such as distraction, restlessness, forgetfulness, difficulty completing tasks, or mental overwhelm can also appear when OCD rituals and repetitive physical behaviours take up too much time and energy.
This is why proper assessment and accurate diagnosis matter. Professionals and care workers need to look beyond what the behaviour looks like and ask what intent is driving it. Is the person organising because it helps them function, or because they feel something terrible might happen if they do not? Is the repetition helpful, or is it a compulsion they feel forced to complete?
Understanding intent helps distinguish ADHD traits from OCD compulsions and supports a more accurate OCD diagnosis, ADHD diagnosis, or dual diagnosis where both conditions are present.
Integrated Treatment Strategies for ADHD and OCD
When ADHD and OCD occur together, treatment needs to look at both conditions rather than treating one in isolation. OCD treatment often focuses on reducing compulsions, intrusive thoughts and anxiety, while ADHD support may focus on attention, impulsivity, planning, emotional regulation and daily structure.
A helpful starting point is understanding the OCD experience itself. OCD thoughts are often ego-dystonic, meaning they feel unwanted, distressing and out of line with the person’s values. This is different from a simple preference for order or routine. A person may know a fear is irrational, yet still feel driven to check, repeat, avoid or seek reassurance to reduce anxiety.
CBT with ERP is one of the most effective treatments for OCD. ERP helps people gradually face feared thoughts or situations while resisting the compulsion that usually follows. Over time, the brain learns that anxiety can rise and fall without needing a ritual to feel safe. The NHS describes CBT with ERP as the usual talking therapy for OCD, and NICE guidance also recommends CBT including ERP as part of OCD treatment.
For ADHD, effective treatment may include psychoeducation, environmental adjustments, routines, skills-based support, coaching, therapy and, for some people, medication. NICE guidance covers ADHD management across children, young people and adults, with support tailored to the person’s needs, age and level of impairment.
An integrated approach may include:
- Accurate assessment to understand whether behaviours are driven by anxiety, impulsivity, executive dysfunction, intrusive thoughts, or a combination.
- CBT and ERP for OCD, adapted so ADHD-related difficulties with focus, planning or consistency do not block progress.
- Practical ADHD strategies, such as reminders, visual routines, shorter therapy tasks and structured follow-up.
- Anxiety support, because anxiety disorders can intensify both OCD rituals and ADHD overwhelm.
- Medication review, where appropriate, especially when symptoms from one condition are worsening the other.
- Support from professionals who understand both conditions, so compulsions are not mistaken for “organisation” and ADHD difficulties are not judged as lack of effort.
The aim is not to make the person “more organised” or simply reduce visible behaviours. Effective treatment helps the person understand what is happening in their mind and body, reduce distress, build safer coping strategies and regain more control over everyday life.
Nurseline Community Services Support People with Complex Mental Health Needs
Living with both ADHD and OCD can feel exhausting and emotionally overwhelming. Many people describe feeling trapped between chaos and control – struggling with racing thoughts, impulsivity, forgetfulness, intrusive fears, or repetitive behaviours that are difficult to stop, even when they know they do not want them. At Nurseline Community Services, support begins by understanding the person’s lived experience, not just the diagnosis.
ADHD and OCD can affect every part of daily life, including routines, relationships, emotional regulation, sleep, work, education, and confidence. What may look like distraction, avoidance, perfectionism, reassurance seeking, or “overthinking” is often linked to a nervous system that feels constantly overwhelmed or stuck in cycles of anxiety and mental fatigue.
- Mental health nurses – offering emotional support during periods of distress, anxiety, intrusive thoughts, and emotional overwhelm, while helping people develop safer and healthier coping strategies.
- Occupational therapy – helping people build manageable routines, reduce overwhelm, improve executive functioning, and regain confidence in daily tasks and independence.
- Trauma-informed support – recognising how past experiences, chronic stress, shame, or long-term masking may affect emotional well-being, safety, and self-perception.
- Multimedia support – using personalised and visual approaches to help people express thoughts and emotions, understand behavioural patterns, and communicate experiences that may feel difficult to explain verbally.
- Recovery-focused support – providing consistency, reassurance, and therapeutic support while helping people better understand how ADHD and OCD interact in everyday life.
If someone is struggling with ADHD and OCD, the right support can make daily life feel more manageable. Through a personalised assessment, we take time to understand the person’s experiences, challenges, strengths, and support needs. From there, tailored care plans are developed to support emotional well-being, independence, stability, and long-term recovery.
Contact us today or make a referral.
FAQs
Can you have ADHD and OCD?
Yes. OCD and ADHD can exist together, and this is more common than many people realise. ADHD often affects focus, impulsivity, and organisation, while OCD is driven by intrusive thoughts and compulsions linked to anxiety. When both are present, symptoms can overlap and make daily life feel mentally exhausting or confusing.
Can ADHD cause OCD?
No, ADHD does not directly cause OCD. However, living with unmanaged ADHD can increase stress, overwhelm, anxiety, and uncertainty, which may intensify obsessive thinking or compulsive behaviours in some people. Both conditions also involve differences in brain functioning and can co-occur.
Can ADHD stimulants make OCD worse?
Sometimes. Increased focus or mental hyperfixation can intensify obsessive thoughts or compulsive behaviours in some people with both Attention-Deficit/Hyperactivity Disorder and Obsessive-Compulsive Disorder. For others, better attention and reduced overwhelm may help them manage OCD symptoms more effectively. Experiences can vary from person to person.


