Key Takeaways
- PBS reduces crises by addressing causes, not behaviour alone
Evidence shows that crises are reduced when unmet needs, triggers, and communication difficulties are understood and addressed early. - Early support is more effective than crisis intervention
Research consistently shows proactive, personalised PBS approaches prevent escalation better than reactive responses. - Calm, consistent responses lower the risk during a crisis
Predictable, non-threatening responses reduce distress and help people regain a sense of safety more quickly. - Long-term PBS leads to fewer and less intense crises
Studies link consistent PBS use with reduced restrictive practices and improved daily stability over time.
It is particularly beneficial for people living with developmental and neurological differences, including autism, learning disability and/or mental health needs.
Real support means getting a closer look at the nature of people’s behaviours. Not only to notice, but to understand and respond in the right way.
What is Positive Behaviour Support (PBS)?
Positive Behaviour Support (PBS) is an evidence-based, person-centred practice aiming to improve quality of life and reduce behaviours of concern by identifying their purpose and function. PBS involves people-centred planning and social validity to create tailored interventions that address each person’s specific needs and preferences.
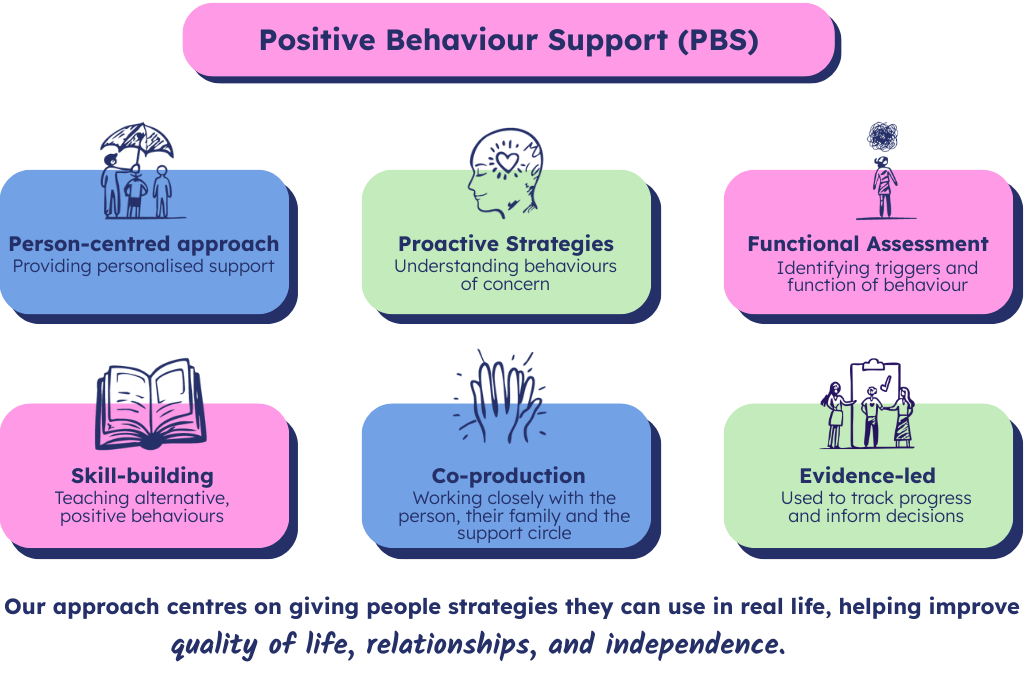
Key aspects of PBS include:
- Understanding the “why”: Taking time to understand what someone is trying to communicate through their behaviour, including sensory needs, communication difficulties, or a need to escape distress.
- Proactive focus: Making thoughtful changes to environments and routines to reduce distress before it builds.
- Skill building: Supporting people to learn practical ways to express their needs and cope more effectively.
- Quality of life: Supporting independence, meaningful relationships, and personal choice in everyday life.
- Shared planning: Working alongside families, carers, and professionals to create support that truly fits the person.
Positive Behaviour Support (PBS) has shown remarkable results in supporting people with disabilities, autism, or mental health needs to live with greater inclusion, independence, and respect.
A crucial aspect of Positive Behaviour Support is its emphasis on collaboration with the person, their family, and other support networks. This collaborative approach ensures that interventions are person-centred and effective, making everyone involved feel included and valued in the process.
- PBS is shown to reduce restrictive practices and repeat crises by focusing on function, not behaviour alone
- Proactive PBS reduces escalation and improves predictability and safety
- Functional understanding and skill development result in fewer and less intense incidents over time
What Are Proactive Strategies?
Proactive strategies within Positive Behaviour Support are designed to prevent challenging behaviours before they occur by addressing the underlying causes and creating supportive environments. These strategies focus on enhancing the person’s quality of life, teaching new skills, and modifying the environment to reduce the likelihood of triggers that may lead to crises.
By anticipating potential issues and implementing preventative measures, proactive strategies aim to minimise the need for reactive interventions – fostering a more stable and positive atmosphere.
Examples of proactive measures include developing individualised support plans that incorporate the person’s strengths and preferences, teaching communication and coping skills, and making environmental adjustments such as reducing sensory overload or providing structured routines.
For instance, if a person becomes agitated in noisy environments, a proactive strategy might involve creating a quiet space where they can retreat when needed. Similarly, if transitions between activities are a trigger, providing clear visual schedules can help ease anxiety and prevent escalation. When care providers implement Positive Behaviour Support, these proactive approaches not only mitigate the risk of crises but also empower people to navigate their environments more effectively and independently.
Proactive vs Reactive Responses
Proactive strategies within Positive Behaviour Support are designed to prevent challenging behaviours before they occur by addressing the underlying causes and creating supportive environments. These strategies focus on enhancing the person’s quality of life, teaching new skills, and modifying the environment to reduce the likelihood of triggers that may lead to crises.
By anticipating potential issues and implementing preventative measures, proactive strategies aim to minimise the need for reactive interventions – creating a more stable and positive atmosphere.
Examples of proactive measures include developing individualised support plans that incorporate the person’s strengths and preferences, teaching communication and coping skills, and making environmental adjustments such as reducing sensory overload or providing structured routines.
For instance, if a person becomes agitated in noisy environments, a proactive strategy might involve creating a quiet space where they can retreat when needed. Similarly, if transitions between activities are a trigger, providing clear visual schedules can help ease anxiety and prevent escalation. When care providers implement Positive Behaviour Support, these proactive approaches not only mitigate the risk of crises but also empower people to navigate their environments more effectively and independently.
How PBS Works in Crisis Situations?
The first step in PBS is understanding people’s behaviour. Behaviours of concern are identified by considering the following factors:
- Is the behaviour harming or limiting the person’s quality of life?
- Is the behaviour causing a risk of harm to the person?
- Is the behaviour causing a risk of harm to other people? Are there restrictions in the person’s life due to the specific behaviour?
After answering these questions and making a personalised PBS plan, the crisis management support is focused on:
- Identifying early signs of distress
PBS focuses on noticing changes in behaviour, communication, and regulation before the crisis escalates. - Detecting triggers and unmet needs
PBS looks at what is driving distress, including environmental, sensory, emotional, and communication factors. - Reducing escalation through proactive support
PBS uses calm, predictable responses that help distress settle and restore a sense of safety. - Protecting safety while respecting dignity
PBS prioritises the least restrictive responses that safeguard wellbeing and human rights. - Strengthen future support through learning
PBS uses each crisis to refine personalised support and reduce future risk.
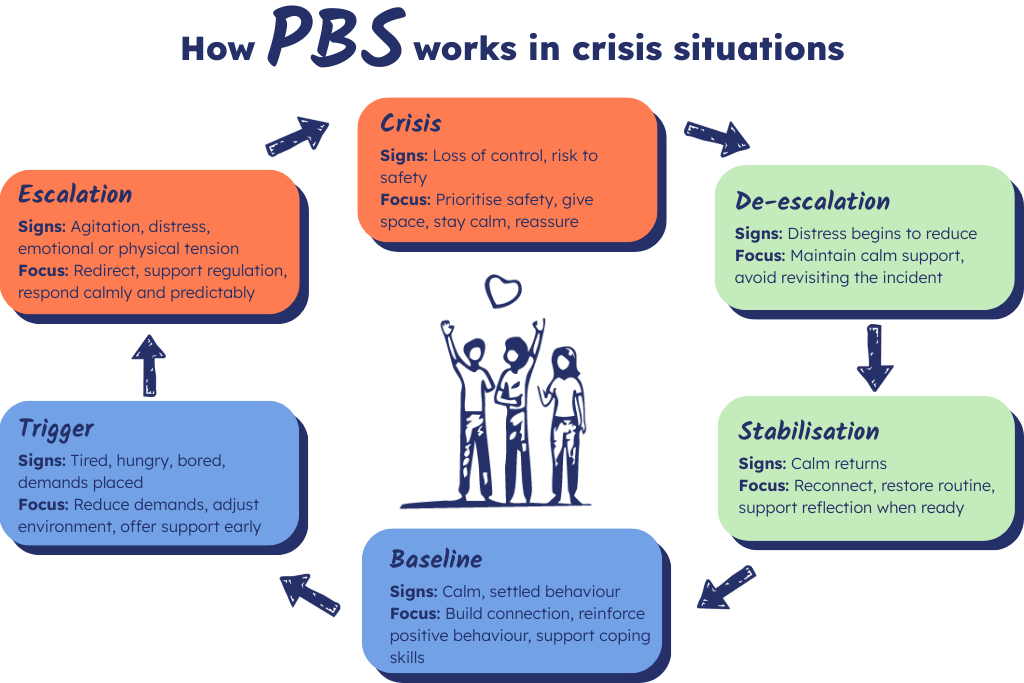
The Escalation Cycle
The escalation cycle is a conceptual framework used to understand and manage the progression of behaviour that challenges. This cycle outlines the typical stages that behaviours go through, from the initial trigger to the eventual stabilisation after a crisis. By recognising and addressing each stage, caregivers and support workers can intervene more effectively to prevent behaviours from escalating and provide the right support.
Trigger
The trigger phase is the initial stage of the escalation cycle, where an event or stimulus sets off a chain reaction leading to challenging behaviour. Triggers can vary widely among people but often include environmental factors, physical discomfort, or emotional stressors. Common examples of triggers include sudden changes in routine, sensory overload, communication challenges, or unmet needs. Identifying and understanding these triggers is crucial for implementing proactive strategies to prevent escalation.
Escalation
During the escalation phase, a person’s behaviour begins to intensify as they react to the trigger. This phase is marked by increasing signs of distress and agitation, which may include verbal outbursts, physical restlessness, or withdrawal. Indicators of escalating behaviour can include raised voice, pacing, clenched fists, or heightened anxiety. The importance of early recognition of these signs cannot be overstated, as it allows for timely intervention to de-escalate the situation and prevent it from reaching a crisis point, fostering a sense of vigilance and proactive response.
Crisis
The crisis phase is characterised by a peak in challenging behaviour, during which the person may become highly agitated, aggressive, or self-injurious. This is the most intense and potentially dangerous stage of the escalation cycle. Managing this phase effectively is critical to ensuring the safety of the person and those around them. Interventions during a crisis should focus on maintaining a calm and controlled environment, using de-escalation techniques, and providing immediate support to the person to help them regain control. Effective crisis management can significantly reduce the duration and severity of the episode and pave the way for a smoother transition to the de-escalation and stabilisation phases.
De-escalation
The de-escalation phase follows the crisis peak and involves calming the person down and reducing the intensity of their behaviour. During this stage, the focus is on using strategies that promote relaxation and help the person regain a sense of control. Techniques such as speaking in a calm and reassuring tone, providing physical space, and using relaxation tools like deep breathing exercises or sensory items can be effective.
The goal of de-escalation is to create a safe and supportive environment that allows the person to gradually transition from a state of high arousal to a calmer and more manageable state. Effective de-escalation requires patience, empathy, and a deep understanding of the person’s needs and triggers.
Stabilisation
The stabilisation phase is the final stage of the escalation cycle, where the person returns to their baseline state of behaviour and emotional regulation. This phase is crucial for ensuring the person feels secure and understood, preventing a rapid recurrence of challenging behaviour. During stabilisation, it is important to continue providing support and reassurance, helping the person process the event and understand what happened.
Interventions in the stabilisation phase might include debriefing sessions, where the person and their support team can reflect on the incident, identify successful strategies, and plan for future prevention. It is also an opportunity to reinforce positive behaviours and skills that were effective during the de-escalation process.
Implementing Positive Reinforcement
Implementing positive reinforcement is a key component of Positive Behaviour Support and involves encouraging desirable behaviours through positive reinforcement.
Positive reinforcement can take many forms, such as verbal praise, tangible rewards, or preferred activities. The aim is to increase the likelihood of the desired behaviour by associating it with positive outcomes. For effective implementation, it is crucial to understand what motivates the person and to deliver reinforcement consistently and immediately following the desired behaviour.
Positive reinforcement should be personalised and meaningful to the person to be effective. For instance, a child might respond well to praise and stickers, while an adult might prefer recognition or extra leisure time. By focusing on reinforcing positive behaviours rather than punishing negative ones, PBS promotes a supportive and encouraging environment that fosters learning and growth.
Positive Outcomes with PBS
Positive Behaviour Support has been shown to lead to significant positive outcomes for people with challenging behaviour. One of the primary benefits is the reduction in the frequency and severity of challenging behaviour, which can lead to a safer and more harmonious environment for both the person and those around them.
Furthermore, PBS improves the quality of life for people by focusing on their strengths and preferences. This person-centred approach ensures that interventions are tailored to the person’s unique needs, promoting autonomy and self-determination.
Additionally, PBS has positive implications for caregivers and support networks. By providing a structured and evidence-based framework for intervention, PBS reduces the stress and burnout often associated with managing challenging behaviour. Caregivers and support workers can feel more confident and competent in their roles, knowing they have effective tools and strategies at their disposal.
What is a PBS Plan?
A Positive Behaviour Support plan is a detailed and individualised strategy designed to address and support a person’s specific behavioural needs. The plan is developed collaboratively, involving the person, their family, and other key stakeholders to ensure it is person-centred and holistic. Positive Behaviour Support plans include a thorough assessment of a person’s strengths, preferences, and triggers, along with specific, proactive strategies to address them.
The plan outlines the positive reinforcement techniques to encourage desirable behaviours, along with detailed interventions for each stage of the escalation cycle. It also includes crisis management protocols to ensure safety and stability during challenging episodes. Regular monitoring and review of the PBS plan are essential to assess its effectiveness and make necessary adjustments based on the individual’s progress and changing needs.
Where Can it Be Used, and Who Should Use it?
Implementing a PBS plan ensures that all interventions are consistent, evidence-based, and tailored to the person’s unique circumstances. It provides a clear roadmap for caregivers and healthcare professionals, promoting coordinated and effective support. By focusing on proactive strategies and positive reinforcement, a PBS plan aims to enhance the person’s life, reduce challenging behaviours, and foster a more supportive and empowering environment.
A Positive Behavioural Support plan can support a range of people with different needs, including people experiencing behaviour that challenges. It is often used to support autistic people and people with learning disabilities. PBS plans can also help people of all ages, from young children to older adults. Its principles are adaptable to various contexts, making it a versatile approach for addressing behavioural challenges in diverse environments.
How Trauma-Informed Practice Strengthens PBS in Crisis
Trauma-informed crisis intervention is an approach that recognises how previous traumatic experiences can shape how someone reacts in a moment of crisis. It places safety, trust, and a sense of control at the centre of the response, understanding that present behaviour may be rooted in past harm. This way of working is relevant across many professional environments – including health and mental health services, personal support roles, crisis teams, and emergency settings – wherever people may be experiencing distress.
A trauma-informed approach begins with curiosity about a person’s experiences rather than judgment about their behaviour. It asks, “What has this person lived through?” instead of assuming something is wrong with them. It recognises that what may be described as challenging behaviour can often be an attempt to cope, adapt, or survive.
At its core, trauma-informed care is about helping someone feel safe enough to breathe again. It’s about responding with patience instead of judgement, especially when behaviour is coming from pain. It means giving people time, steadiness, and real support to learn how to calm their body, understand their reactions, and feel more in control of their days. It’s not theory. It’s how we treat people when they are at their most overwhelmed.
PBS Support with Nurseline Community Services
Nurseline Community Services provides nurse-led, personalised support at home. With an experienced team of PBS specialists, mental health nurses, multimedia and communication specialists, we provide urgent crisis support in the right place and at the right time.
Our team of skilled and experienced PBS practitioners brings years of expertise in health and social care. We work collaboratively, drawing on each team member’s strengths, knowledge, and experience to deliver the best possible support. Our areas of expertise include:
- Supporting people to move smoothly and safely from hospital settings into the community.
- Supporting people with multiple physical and neurodevelopmental differences who require a high level of support to live a fulfilled life in the community.
- Preventing unnecessary inpatient admissions or readmissions for people with significant support needs.
- Designing living environments to meet the needs of people who display behaviours of concern.
- Minimising or removing restrictions, using them only as a last resort.
- Trans-disciplinary working within complex situations.
- Multi-media planning and support.
In dealing with crisis situations, we employ a highly trained rapid response team available 24/7 to provide immediate and effective intervention. Our team is skilled in de-escalation techniques and crisis management, ensuring the safety and well-being of everyone involved. We work collaboratively with people, their families, and other support networks to develop comprehensive PBS plans that address both immediate and long-term needs.
Our commitment to excellence and personalised care makes us a trusted partner in managing challenging behaviours. To learn more about how we can support you or your loved one with PBS, contact us today.
Let us help you create a positive and supportive environment that fosters growth and well-being.