Neurodevelopmental differences like attention-deficit hyperactivity disorder often co-occur with certain mental health conditions, including eating disorders. Numbers show that around 12% of people with ADHD also happen to have an eating disorder, with binge eating disorder being the most frequent. Yet, the co-occurring incidence of bulimia nervosa and anorexia nervosa is not excluded as well.
Are eating disorders related to attention deficit hyperactivity disorder?
While many people experience at least one form of eating disorder in their lifetime, people with ADHD may experience ongoing challenges with regulating appetite and controlling impulses related to food.
- People with ADHD are around three times more likely to develop an eating disorder compared with the general population.
- Some studies estimate that about 20% of children with ADHD develop an eating disorder later in life.
- Girls with ADHD were found to be 3.6 times more likely to develop any eating disorder and 5.6 times more likely to develop bulimia nervosa.
When ADHD is recognised and treated early, many of the drivers of disordered eating (impulsivity, emotional dysregulation, stress eating) can be addressed before they develop into a full eating disorder.
Why ADHD and Eating Disorders Often Occur Together?
ADHD and eating disorders often appear together because they share several underlying psychological and neurological mechanisms. Research increasingly shows that difficulties with impulse control, emotional regulation, and reward processing – all commonly associated with attention-deficit hyperactivity disorder – can influence eating behaviours and shape the way people relate to food, increasing vulnerability to conditions such as binge eating disorder, bulimia nervosa, and sometimes anorexia nervosa.
Numbers indicate that people with ADHD are up to three times more likely to develop an eating disorder, and around one in five children with ADHD may experience disordered eating behaviours. Early diagnosis and support can therefore play a powerful role in preventing these patterns from becoming long-term health problems
The Prevalence of ADHD in People with Eating Disorders
Research over the past decade has consistently shown that ADHD and eating disorders occur together more often than many people realise. Studies suggest that between 5% and 17% of people receiving treatment for an eating disorder also experience ADHD symptoms, a rate significantly higher than in the general population.
When looking at specific eating disorders, the overlap becomes even clearer: ADHD has been reported in 3–16% of people with anorexia nervosa, 9–35% of people with bulimia nervosa, and around 20% of people with binge eating disorder. Large reviews also show that people with ADHD are about 3-4 times more likely to develop an eating disorder compared with people without ADHD.
These patterns have encouraged researchers to look more closely at how neurodevelopmental differences influence eating behaviours, emotional regulation, and everyday routines around food.
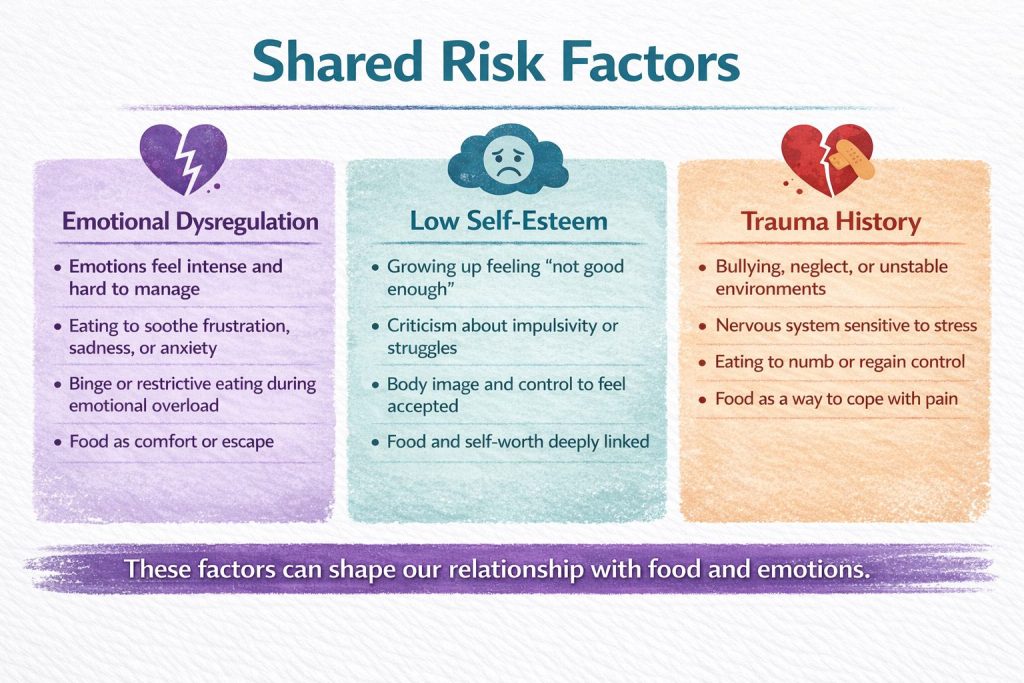
Shared Risk Factors
People living with ADHD often describe emotional experiences that are intense, fast-moving, and sometimes difficult to regulate. When these experiences intersect with eating behaviours, certain shared vulnerabilities can appear.
Emotional dysregulation
- Emotions may rise quickly and feel overwhelming, making it difficult to pause or regain balance.
- Eating can become a way to calm intense feelings such as frustration, sadness, boredom, or anxiety.
- Some people describe binge eating or restrictive eating patterns emerging during moments of emotional overload.
- Food may temporarily create comfort, distraction, or relief when emotions feel difficult to manage.
Low self-esteem
- Many people with ADHD grow up hearing criticism about impulsivity, organisation, or academic struggles.
- Repeated experiences of feeling “not good enough” can slowly shape self-worth.
- Body image or control over food may become areas where someone tries to regain confidence or acceptance.
- Eating patterns can sometimes reflect deeper struggles with self-perception and identity.
Trauma history
- People with ADHD are more likely to report experiences such as bullying, emotional neglect, or unstable environments.
- Trauma can leave the nervous system highly sensitive to stress and emotional triggers.
- Eating behaviours may develop as coping strategies – ways to numb distress, create control, or escape painful memories.
- For some, food becomes one of the few accessible ways to manage overwhelming feelings.
Together, these experiences do not cause eating disorders on their own, but they can shape a person’s relationship with food, emotions, and self-worth over time.
What Drives the Link Between ADHD and Eating Disorders?
Many people living with ADHD describe long-standing challenges with:
- Impulsivity, which can make it harder to pause before eating or to stop once eating has started
- Emotional dysregulation, where food may become a quick way to soothe stress, frustration, or overwhelm
- Difficulty maintaining routines, including irregular meal patterns or skipping meals unintentionally
- Sensitivity to reward and dopamine, which can make highly palatable foods especially appealing
- Periods of hyperfocus, where eating is forgotten for hours and followed later by intense hunger
- Executive functioning challenges, affecting planning meals, grocery shopping, or organising regular eating patterns
- Heightened stress or sensory sensitivities, which may influence food choices, textures, or eating environments
Executive Function Difficulties
Many people with ADHD describe everyday tasks like planning meals or meal preparation as more complicated than they appear from the outside. Executive functions – skills that help with organising, planning ahead, and making decisions – can be harder to manage. As a result, eating routines may become irregular. Meals might be forgotten, delayed, or pushed aside while attention moves to something else.
By the time hunger is noticed, it may already feel intense and urgent.
In those moments, the body is simply trying to catch up. Eating quickly or consuming large amounts of food can happen after long periods without eating. Making decisions about what to cook, finding ingredients, or organising a meal can also feel mentally exhausting, especially on days when concentration is already stretched thin. Over time, this can create a pattern where eating feels chaotic.
In most cases, daily planning and decision-making require much more effort than people often realise.
Impulsivity, Reward, and the Dopamine Factor
Impulsive eating can sometimes be part of life with ADHD. A craving may show up suddenly, and eating can happen almost automatically – especially when food is right there. In that moment, food can feel like a quick fix, a simple way to take the edge off restlessness, boredom, emotional tension, or mental exhaustion. It isn’t always about hunger. Sometimes it’s just about trying to feel a little better, even if only for a short while.
Behind this is the way dopamine and the brain’s reward pathways work in ADHD. When dopamine levels fluctuate, the brain naturally looks for things that bring a quick sense of relief or satisfaction. Certain foods can trigger that response and provide a brief feeling of comfort or pleasure. The difficulty is that the effect fades quickly. When it does, the urge to reach for that same feeling can return again, which can gradually lead to patterns of impulsive eating and binge cycles.
Often, it reflects a brain trying to regulate itself rather than a lack of control.
Emotional Factors and Self-Esteem
Our emotional state can sometimes be directly connected to how we experience eating. People with ADHD are no exception. In moments of emotional dysregulation, feelings can rise quickly and feel difficult to control, and in these moments, food may become a way of coping.
Emotional eating – using food to manage stress, sadness, loneliness, or overwhelm – can bring a brief sense of relief. At the same time, some people move in the opposite direction and develop restrictive eating habits, trying to limit or control food as a way to regain a sense of control when emotions feel chaotic.
Over time, these experiences can start to affect how a person feels about themselves. Episodes of emotional eating or periods of restriction may be followed by shame, self-criticism, or a quiet sense of low self-worth.
Interoception and Body Awareness
The body usually sends quiet signals to let us know when it needs food or when it has had enough. For people with ADHD, these signals can sometimes be harder to notice. Hunger cues may be ignored or simply missed, especially when attention is absorbed in work, conversations, or screens. Hours can pass before the body’s need for food becomes clear. At other times, eating can happen almost on autopilot, particularly when there are distractions around.
In those moments, overeating due to distraction can occur because the body’s signal of fullness doesn’t fully register.
Food can also become a way of finding balance during emotional moments. Some people notice themselves eating to regulate emotions, reaching for something comforting when stress, restlessness, or overwhelm builds up. Over time, these patterns can affect the body in different ways. Skipping meals or not noticing hunger may contribute to low body weight, while repeated distracted or emotional eating may lead to gaining weight.
In many cases, the challenge is not about discipline or willpower – it is about learning to reconnect with the body and gently recognising the signals it has been sending all along.
Sleep and Other Behavioural Factors
Sleep and daily routines can quietly shape the way eating happens throughout the day. For people with ADHD, sleep is often irregular – nights may stretch later than intended, mornings may start rushed, and the body’s rhythm around hunger can become unpredictable.
When sleep is disrupted, appetite can shift as well. Some mornings, there is little interest in food, while other times the body begins craving quick energy later in the day. Long hours of screen time, especially late at night, can also make it harder for the body to settle into a steady sleep and eating rhythm.
These everyday patterns can influence food in several ways:
- Irregular routines can make regular meals harder to maintain
- Sleep difficulties may leave the body feeling drained and searching for quick energy
- Late-night screen time can delay sleep and sometimes lead to evening snacking
- Sensitive or picky eating can make certain textures, smells, or tastes feel overwhelming
- Changing appetite during the day, with little hunger earlier and stronger hunger later on
Over time, sleep, routine, and eating patterns become closely connected. When the body lacks rest or structure, food choices can become more reactive and less predictable. For many people, it is not about a lack of effort – it is simply the body trying to keep up with an already demanding rhythm.
How ADHD and Eating Disorders Can Look in Real Life?
The connection between ADHD and eating difficulties does not always look obvious from the outside. It often shows up in small, everyday moments – skipped meals during busy days, eating quickly after long hours without food, or turning to food during emotional overwhelm. For some people, eating becomes irregular and unpredictable, shaped by distraction, impulsivity, and shifting energy levels. Understanding these experiences in real life helps move the conversation away from blame and closer to compassion.
ADHD and Binge Eating or Overeating
In everyday life, eating patterns in ADHD can become irregular without someone fully realising it. Missed meals, intense hunger later in the day, or eating while distracted can sometimes lead to binge eating, compulsive eating, and over time gaining weight. These patterns often grow from impulsivity, fluctuating energy levels, and the brain’s search for quick comfort or stimulation.
Example 1 – The “missed meals” cycle
A person becomes absorbed in work or a task and forgets to eat for hours. By the evening, hunger feels overwhelming. Food is eaten quickly and in large amounts because the body is trying to catch up after a long gap without food.
Example 2 – Eating for comfort after emotional overwhelm
After a stressful or emotionally draining day, food becomes a way to calm down. Eating brings a short moment of relief, but the urge can return again later, sometimes turning into compulsive eating over time.
ADHD and Restrictive Eating
Restrictive eating can also appear in people with ADHD, though it is often overlooked. Instead of eating too much, the challenge may be not eating enough. Hunger cues may be missed, meals may feel like an interruption during periods of focus, or the effort of planning and preparing food can feel overwhelming. Over time, these patterns can lead to low body weight and low energy, even when the person never intended to restrict food intake.
Example 1 – Losing track of meals
Someone becomes deeply focused on work, studying, or a hobby and hours pass without noticing hunger. By the time the body signals the need for food, the person may feel too tired, distracted, or uninterested to prepare a full meal.
Example 2 – Food feels overwhelming
Planning what to eat, preparing ingredients, and making decisions about meals can sometimes feel exhausting. Instead of going through the whole process, the person may skip meals or eat very small amounts, gradually leading to low body weight.
Getting a Diagnosis: What to Look For
For some people, it takes years before anyone connects the dots between ADHD and eating struggles. Eating may feel unpredictable – some days forgetting meals completely, other days eating far more than intended, without really understanding why it keeps happening.
It can be confusing and sometimes frustrating to live with these patterns without a clear explanation. When these experiences appear alongside difficulties with focus, routines, impulsive decisions, or strong emotional reactions, it may begin to suggest that ADHD could be part of the story.
Signs You Might Have Both ADHD and an Eating Disorder
For some people, the story starts long before eating difficulties appear. There may have been signs of childhood ADHD – a mind that wandered in class, unfinished homework, constant restlessness, or feeling different from others. Years later, struggles with food may begin to show up as well. This pattern is often seen in adolescent girls, where ADHD can remain unnoticed while concerns around eating, weight, or body image slowly take centre stage.
You might recognise some of these experiences:
- Looking back and realising ADHD traits were present since childhood
- Eating that feels out of balance – sometimes skipping meals, other times overeating
- Food becoming a way to deal with stress, overwhelm, or difficult emotions
- Finding it hard to keep regular routines around meals and daily structure
- Feeling ashamed, confused, or frustrated about eating habits or body shape
For many people, these patterns only begin to make sense once both ADHD and eating difficulties are considered together.
ADHD and Forgetting to Eat
Is forgetting to eat a sign of ADHD?
It can be. When someone with ADHD becomes deeply focused on something – work, studying, or even a hobby – hunger can easily be pushed aside. Hours may pass before the person suddenly realises they haven’t eaten all day. It’s not intentional; attention is simply elsewhere, and the body’s signals are noticed much later.
Treatment Approaches for Co‑Occurring ADHD and Eating Disorders
The way attention shifts, emotions rise, routines break down, and hunger signals get missed all play a role. From there, treatment focuses on helping someone make sense of their patterns with food, attention, and emotions, while gradually finding ways that feel more manageable and supportive in daily life.
What ADHD‑Informed Eating Disorder Treatment Looks Like?
Recovery usually starts with slowing things down and trying to understand what a person has been going through. Support is not only about changing eating habits, but about understanding the experiences behind them.
- Assessment – taking time to explore what may be driving the eating difficulties. This includes looking at ADHD traits, emotions, routines, eating patterns, and everyday challenges to understand what the person has been struggling with.
- Creating personalised support – once there is a clearer picture, support can be shaped around the person’s own experiences, emotional struggles, and strengths. What helps one person may look very different for someone else.
- Recognising possible trauma – gently exploring whether past experiences may be influencing the person’s relationship with food, emotions, or self-worth.
- Walking alongside the recovery process – recovery is rarely quick or straightforward. What often helps most is consistent, patient support, built on trust, understanding, and the feeling that someone is truly there through the ups and downs.
Therapies That Can Help
Several therapeutic approaches can support people experiencing both ADHD and eating disorders. Some commonly used therapies include:
- Cognitive Behavioural Therapy (CBT) – helps people recognise patterns between thoughts, emotions, and eating behaviours and develop healthier coping strategies.
- Dialectical Behaviour Therapy (DBT) – focuses on managing strong emotions, reducing impulsive behaviours, and building emotional regulation skills.
- Trauma-informed therapy – explores how past difficult experiences may influence emotions, self-worth, and relationships with food.
- Group therapy – provides a safe space to share experiences with others facing similar struggles, helping reduce shame and isolation.

Support with Nurseline Community Services
Recovery can feel confusing and lonely when someone is living with both ADHD and eating difficulties. At Nurseline Community Services, support begins by listening carefully to the person’s story and understanding what daily life has really been like for them. Eating struggles are rarely just about food. They are often connected to emotions, past experiences, routines, and the way the ADHD mind processes stress and overwhelm.
- Mental health nurses – offering emotional support during difficult moments and helping people work through anxiety, distress, and overwhelming thoughts that may influence eating patterns.
- Occupational therapy – helping people rebuild daily routines, develop healthier habits around meals, and regain confidence in everyday activities.
- Trauma-informed support – recognising that past experiences may shape how someone relates to food, emotions, and their sense of safety.
- Multimedia support – using visual and personalised tools to help people express feelings, understand their experiences, and learn new coping strategies.
- Recovery-focused support – walking alongside people throughout their recovery journey, offering consistency, understanding, and encouragement as they rebuild a healthier relationship with food and themselves.
If you or someone you support is struggling with ADHD and eating difficulties, the right support can make a real difference. Through a personalised assessment, we take time to understand the person’s experiences and what may be contributing to the eating challenges. From there, we develop tailored care plans that support recovery, emotional well-being, and everyday stability.



